Others
GOVERNANCE REFORMS IN MEDICAL EDUCATION (2014-2020)
प्रविष्टि तिथि:
16 DEC 2021 13:37 PM
REFORM, PERFORM, TRANSFORM
(Ministry of Health & Family Welfare)
December 16, 2021
1. Introduction
Regulatory reforms brought in the sector of Medical Education over the last six years have transformed this sector, bringing in transparency, meritocracy and expansion. India is well on the path of becoming a leader in health care delivery.
2. Background
- Mudaliar committee (1961) suggested establishing one medical college for a population of 50 lakhs and advocated for a Doctor:Population ratio of 1:3000.
· The World Health Organization (WHO) currently recommends a Doctor:Population ratio of1:1000.
- In India, shortfall of medical human resources was a major challenge. The problem was not only limited to the numbers, but there were challenges in distribution and quality as well. Availability, Accessibility and Quality - all needed focus.
3. The Situation in 2014: Need for Reforms
- While India had a limited number of 381 medical colleges in 2014, the system was riddled with far too many problems.
· The overarching regulatory body of the medical colleges, the Medical Council of India (MCI) had become ‘a high entry barrier'. This had led to paucity in the number of medical colleges and number of seats, both at the undergraduate and the post graduate levels, across the country.
· All functions and authority related to medical colleges was concentrated and centralized in the Medical Council of India, making it unwieldy, slow and inefficient in decision making.
· Many medical colleges, especially in the private sector, suffered from low-quality education and high fees.
· District hospitals and large private hospitals remained unutilized for teaching purposes.
· There were multiple entrance examinations for undergraduate and post graduate courses.
· In many private colleges, the admission was on the basis of capitation fee and not merit.
- The regulatory norms prohibited expansion of medical colleges.
4. Institutional Reform: National Medical Commission
- The biggest step of the Central government after 2014 has been the establishment of the National Medical Commission (NMC).
· This was achieved by passing of the National Medical Commission Act in August 2019, which came into force on 25thSeptember 2020.
· NMC will make the medical education in India quality-oriented, competency-based, equitable, affordable and at par with the best in the world.
- Four mutually independent and autonomous boards have been created which would work under the overall supervision of the National Medical Commission. These are:the Under-Graduate Medical Education Board, the Post-Graduate Medical Education Board, the Medical Assessment and Rating Board, and the Ethics and Medical Registration Board.
The National Medical Commission has been established to:
- Improve access to quality and affordable medical education
- Ensure availability of adequate and high-quality medical professionals in all parts of the country
- Promote equitable and universal healthcare that encourages community health perspective and makes services of medical professionals accessible to all
- Encourage medical professionals to adopt latest medical research in their work and to contribute to research
- Objectively assess medical institutions periodically in a transparent manner
- Maintain a Medical Register for India
- Enforce high ethical standards in all aspects of medical services
- Have an effective grievance redressal mechanism.
5. Ensuring Availability of Doctors and Specialists: Increase in Number of Medical Colleges
- There have been concerted efforts over the last six years to increase the number of medical colleges. A Centrally Sponsored Scheme was introduced in 2014 to provide central funding support for opening new medical colleges.
- Three phases of the Scheme have been approved till date, under which 157 colleges have been sanctioned. Of these, 47 colleges have already become functional.110 are expected to be functional in next few years.
- Among these, 39 medical colleges are in the Aspirational Districts, where there is acute need for doctors and specialists.
- Against 381 medical colleges in 2014, there are 562 medical colleges today, i.e. an increase of 48 per cent. The number of Undergraduate (UG) seats have increased by 56 per cent and the number of Postgraduate (PG) seats have increased by 80 per cent as compared to 2014.
Pradhan Mantri SwasthyaSuraksha Yojana (PMSSY)
The PMSSY is based on ensuring the three Es of Expand-Equity-Excellence.
Key features of PMSSY
- The scheme aims at correcting regional imbalances in the availability of affordable and reliable tertiary healthcare services and augmenting facilities for quality medical education in the under-served States.
- A total of 21 new All India Institute of Medical Sciences (AIIMS) have been started, out of which MBBS classes have commenced in 18 AIIMS.
6. Quality: Promoting High Standards
- Skill Lab: The new standard for opening of medical colleges envisages a skill laboratory in every medical institution. Here students can practice and improve their skills in safe environment, mitigating the limitations of learning on live Patients.
- New competency-based curriculum: ‘Competency-based Undergraduate Curriculum for the Indian Medical Graduate' has been introduced. The curriculum has been changed after 21 years; previous edition being that of 1997. Another new element is the introduction of elective subjects. Now students can pick up subjects of their choice. Time has been allotted for self-directed learning and co-curricular activities.
- Emergency Medicine Department: All the medical colleges will have emergency medicine department by 2022. The department will have a casualty area, an intensive care unit, an operation theatre and trained staff.
7. Affordability
Regulation of Fee: Before the NMC Act, there was no legal mechanism to regulate the fee charged by the private colleges. The National Medical Commission (NMC) Act has the provision to regulate fee and all other charges in 50 per cent of the seats in private medical colleges and deemed universities. NMC is framing guidelines in this regard.
8. Meritocracy: One Country, One Exam
- NEET: In 2016, a common entrance test- National Eligibility cum Entrance Test (NEET) was introduced, which ensured 'One country, One examination, One merit' system and a common counselling system. This allowed students from anywhere in India an opportunity to study in any medical college in the country based on merit.
- National Exit Test (NEXT): To gauge the standards of competence and knowledge of students passing the MBBS exam, NEXT has been proposed under the NMC Act. This will be a common final year MBBS exam which would not only serve as a licentiate exam for practice, but also serve as an entrance exam for admission to Postgraduate in broad specialty medical courses. Further, the same exam will serve as a screening test for foreign medical graduates.
- Common Counselling: Instead of prevailing practice of separate counselling sessions for different medical colleges, a common counselling at Central level and State level has been started from 2016. This has ensured transparency in admissions.
- Family Medicine: The post graduate program in Family Medicine will produce specialist family physicians. The Family Medicine incorporates the basic knowledge of medicine, surgery, obstetrics and gynecology.
- Community Health Providers: The MBBS and postgraduate doctors prefer to work in cities, creating a vacuum in the rural and peripheral areas. Also, at the primary and promotive healthcare level, many of the services may not require a full-fledged doctor. The NMC Act, therefore, provides for Community Health Providers (CHPs), who would be the health providers connected with modern scientific medical profession with limited right to practice medicine and prescribing medicine in primary and preventive care.
- District Residency Scheme: A Scheme for three-month training for the second/third year Postgraduate medical students at District Hospitals as an essential component of postgraduate medical training curriculum has been introduced.
9. Access in Rural and Peripheral Areas
- Location of Medical Colleges: Equity in medical education and of geographic balance in availability of medical care is being addressed by locating new medical colleges in backward districts. Of the 157 new colleges that are being opened under the Centrally Sponsored Scheme, 39 are coming up in the Aspirational districts.
- Diploma Courses by NBE: In order to meet the shortfall of specialists, the National Board of Examinations (NBE) has launched two-year diplomas in eight disciplines. They have been specifically chosen to meet the public health needs of the country, namely - Anesthesia, Gynecology and Obstetrics, Pediatrics, ENT, Ophthalmology. Family Medicine, Tuberculosis and Chest Diseases and Radio diagnosis.
Progress in NBE Courses (Number of PGs)
|
|
2017
|
2020
|
|
Super Speciality
|
899
|
1779
|
|
Broad Speciality
|
5619
|
7771
|
NBE Accredited Seats and Hospitals
|
Government PSUs/Defence/Hospitals
|
104 accredited hospitals
|
1738 seats
|
|
District/Civil Hospitals
|
64 accredited hospitals
|
457 seats
|
|
Private Hospitals
|
536 accredited hospitals
|
- ts
|
10. National Board of Examinations (NBE)
One important measure to quickly upscale the number of postgraduate seats is through a focus on the NBE. NBE is an autonomous body of the Ministry of Health &Family Welfare for Examination and Accreditation. It accredits the hospitals (mainly private hospitals) for broad specialty and super specialty courses that are equivalent to MD/MS or DM/MCh respectively. Further, the NMC Act has provided suomoto recognition to all courses run by NBE. The NBE has so far accredited 704 hospitals with 9779 seats, 80 per cent of which is in the private sector.
Streamlining Minimum Standards Requirement (MSR) for establishment of Medical Colleges
|
|
Bed requirement (150 seats)
|
Faculty requirement (150 seats)
Faculty Resident
|
|
Before 2015
|
750
|
152
|
115
|
|
2015
|
650
|
132
|
85
|
|
2018
|
650
|
132
|
80
|
|
2020 (New standards)
|
600
|
116
|
76
|
Land Requirement for Establishment of Medical College
|
|
Earlier
|
New Standards
|
|
General
|
20 acres
|
- No minimum land requirement prescribed.
- In Tier1 and 2 cities, Hilly and North East states, two parcel of land within 10 km distance.
- Sharing of teaching spaces by departments.
- Minimum space requirements for functional areas (eg. labs, libraries etc.)rationalised.
- All teaching spaces to be e-learning enabled.
|
|
Class A cities with 25 lakhs+ population and North-East /Hill states.
|
20 acres can be in two parcels within 10km distance, main parcel housing, hospital, college etc cannot be less than 10 acres.
|
|
Metropolitan
|
10 acres
|
11. Reform in Regulations
Besides the increase in number of medical colleges, a number of regulatory reforms were undertaken to streamline the number of UG and PG seats. More than 50 crucial long pending regulatory reforms were brought in the last six years.
Ensuring Availability of Doctors and Specialists
Key Regulatory reforms
- Norms for setting up of a Medical College relaxed.
- Consortium allowed to establisha Medical College.
- Allowing permission for lesser number of seats, if criteria for higher number of seats not met.
- Teacher:Student ratio has been relaxed in PG Regulation.
- Equivalence of Diplomate of National Board (DNB) with PG as faculty.
- Mandatory to start PG in three years from MBBS recognition.
- Permission to apply for PG earlier-at the time of 2nd renewal.
- Intensive Care Unit (ICU) beds to be counted as general beds.
- Starting Super-specialty Department directly within broad specialty.
12. Impact and Outcomes
The reforms and the new/restructured schemes in medical education undertaken in last six years have yielded extraordinary results. Steps taken have not only led to significant increase in the number of the colleges but also a huge increase in the number of seats at both undergraduate and post graduate levels.
|
Outcome of last six years
|
|
|
2014
|
2020
|
Percentage Increase
|
|
Number of Medical colleges
|
381
|
562
|
48
|
|
Number of UG seats
|
54348
|
84649
|
56
|
|
Number of PG seats
|
30191
|
55595
|
80
|
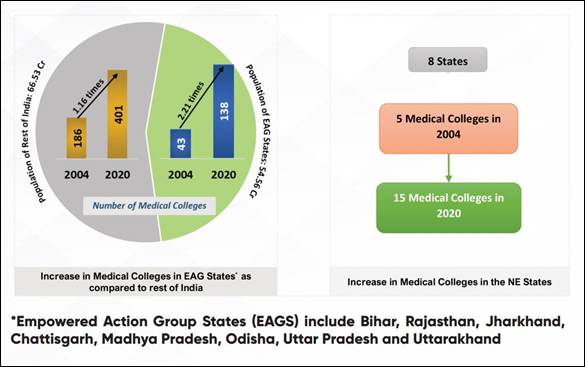
In last six years the location of the new medical colleges has been selected carefully to address the issues of regional equity.
13. The Journey of Reforms Continues
- All these reforms in medical education will have long term impact on primary, secondary and tertiary care in India.
· Reforms will result in one lakh MBBS seats and 65,000 postgraduate seats by 2022.
· The key area in which reforms will continue is quality of education.
· Towards this end, the NMC will ensure effective implementation of competence-based curriculum in all the medical colleges, along with focus on skill-based teaching.
· Parallelly, reforms are ongoing in the sectors of Nursing Education, Dental Education and Allied and Healthcare professions.
· A new Allied and Healthcare Professions Bill - the National Commission for Allied and Healthcare Professional Bill, 2020 had been introduced in the Parliament.
- This shall enable constitution of a National Commission and State Councils to regulate more than 50 diverse allied and healthcare professions. Similarly, on the lines of the NMC, the Dental Council of India and the Indian Nursing Council are also being reformed through new laws.
Source: PIB e- booklet on Reform, Perform and Transform
AG/HP/AKP/SK
(तथ्य सामग्री आईडी: 148592)
आगंतुक पटल : 535
Provide suggestions / comments